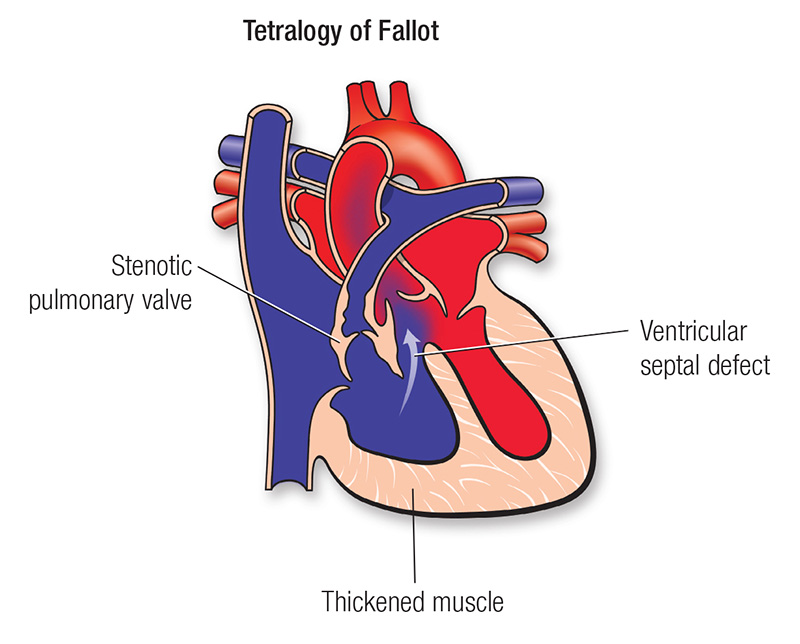
Interactive learning modules for congenital heart disease with lesion-specific diagrams, pulmonary hypertension physiology, and clinical pearls designed for trainees.
Main Author:
Dr. Corey Chartan
Chief of Pulmonary Hypertension
Medical Director, Dell Children's Center for Pulmonary Hypertension
Pediatric Critical Care / Pulmonary Hypertension / ECMO
Dell Children's Medical Center
Associate Professor of Pediatrics
Dell Medical School, The University of Texas at Austin
Austin, Texas
corey.chartan@austin.utexas.edu
Contributors:
Dr. Taylor Saley
Associate Medical Director, Dell Children's Center for Pulmonary Hypertension
Pediatric Cardiology / Pulmonary Hypertension
Assistant Professor of Pediatrics
Dell Medical School, The University of Texas at Austin
Dr. Sowmith Rangu
Heart Failure and Cardiac Intensivist
Assistant Professor of Pediatrics
Dell Medical School, The University of Texas at Austin
Dr. Constantine Mavroudis
Pediatric and Congenital Heart Surgeon
Assistant Professor of Cardiovascular and Thoracic Surgery
Dell Medical School, The University of Texas at Austin
Dr. Sandhya Ramlogan
Medical Director of Echocardiography
Pediatric Cardiology
Associate Professor of Pediatrics
Dell Medical School, The University of Texas at Austin
Claire Champion
PH Nurse Practitioner
Dell Children's Center for Pulmonary Hypertension
Dell Medical School, The University of Texas at Austin
Lisa Musembi
PH Pharmacist
Dell Children's Center for Pulmonary Hypertension
Dell Medical School, The University of Texas at Austin
Disclaimer: This website is for educational purposes only and is not intended to provide medical advice, diagnosis, or treatment. All clinical decisions should be made by qualified healthcare professionals.
Please begin by completing the pre-test assessment. After reviewing the material, proceed to complete the post-test.